Prosthetics
Prosthetic Limb Checkout
Often, after an amputee has been fitted with a prosthesis, they are seen by Physiotherapists for gait training to learn to use it correctly. This can occur with a new amputee with their first limb, or experienced amputees to either correct bad habits or learn to gain the most from new components. When seeing the amputee in any of these situations, the first thing the Physiotherapist should do is perform a prosthetic checkout, that is, examine the fit, alignment and functioning of the prosthesis to make sure it can be used during training without risk to the amputees stump or skin, or risk of falls. If potential problems are found, some can be remedied on the spot, such as adding extra socks in a loosely fitting socket, while others must be referred back to the Prosthetist for correction.
The following steps describe how to perform a checkout, and what to look for.
- General
- Sitting
- Standing
- Suspension
- Walking
- Actions
General
Before donning the prosthesis for the checkout, check the stump for any wounds, abrasions, blisters, areas of redness or discolouration, excessive bony protuberances or scars. This is to assess the baseline condition, so any effects the prosthesis have on the stump and skin can be noted. Also check for contractures in the hip / knee that may need to be accounted for.
Then checkout the prosthesis, beginning before the patient has donned it:
- Is the prosthesis constructed of the components that were prescribed at the clinic?
- Check that all screws and adaptors are tightened, and there are no loose parts
- Is the interior of the socket free from ridges or excessive bulges or areas of coarseness?
- Check that the footwear is firmly on the foot, and not too loose or excessively worn
- Does bench alignment look satisfactory? A rough guide for transtibial prostheses is that they should be able to stand unsupported on flat surfaces. Transfemoral prostheses can also sometimes be expected to stand upright unsupported. For quadrilateral sockets, ensure the posterior brim is parallel to the ground.
- Do articulated components move as expected, without noise?
Ask the amputee to don their prosthesis.
A small ball of plasticine or other compressible material taped to the distal stump (outside the socks / liner) is often useful to help assess the degree of distal contact when the amputee stands, later in the assessment.
- Can the prosthesis be donned relatively easily, including socks and liners, belts and cuffs?
- Take into account the amputees level of experience. If the Physiotherapist needs to assist, the prosthesis should still fit onto the stump fairly easily
Sitting
Ask the amputee to remain sitting, hips and knees around 90 degrees. There may be some differences in what to assess, depending on the level of amputation and the type of prosthesis. TTA refers to Transtibial Amputees; TFA refers to Transfemoral Amputees.
- Can the amputee sit comfortably with hips and knees approximately 90 degrees, feet flat on the floor? Ideally the amputee should be sitting in a chair or on a firm plinth, not their wheelchair or soft bed, where the surface or seat slope may affect their ability to sit upright.
- TTA: If the knee cannot be flexed to 90, it may be that the popiteal brim is too high, or hamstring relief insufficient
- TTA: The liner should not pull out of the socket as the knee flexes to 90 degrees
- TFA: If the amputee cannot sit forward, it may be that the anterior superior brim of the socket is too high, limiting hip flexion
- TFA: Is the thigh segment length such that the knee sits level with the intact knee? Remember to take into account long stump lengths, where it is not possible to align the knees exactly.
- TFA: Does the knee flex, or remain extended? A foot that pokes out may indicate extension assist or flexion damping is too high.
- Assess subjectively & objectively for any areas of pain, or where pressure may be excessive
- TTA: Question and palpate for excessive pressure over the hamstring insertions
- TTA: There should not be any discomfort over the anterodistal tibia. If there is, it may be that the socket is too tight distally, or there is insufficient moulding in the popliteal area, allowing 'gapping' between the superior socket and knee, or the knee to extend inside the socket, pushing the distal tibia forwards.
- TTA: The prosthesis should be on firmly, and not slide distally if the amputee lifts their foot by flexing at the hip
Standing
When performing a checkout in standing, remember that the initial goal is to assess the fit and alignment of the prosthesis, rather than the amputees balance or ability to weightbear, especially with new amputees trialling their first prosthesis. Hand support should be allowed as appropriate, because you really want the amputee to be able to stand erect, without fear or pain. Aim for the best possible posture with minimum possible hand support, feet parallel and a comfortable width apart. Encourage equal weight distribution, as much as possible.
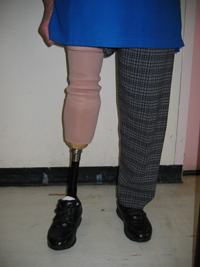
- Question the amputee about excessive discomfort or pain, gathering information on the type, severity and location. These sites should be noted and the stump condition reassessed to gauge if the pressure on stump and skin was excessive or potentially damaging. Some discomfort may be expected in certain situations, which are not necessarily cause for alarm:
- If the amputee normally has a painful stump without the prosthesis
- If they are a new amputee and are unfamiliar with having pressure on surfaces that were not previously used for weight bearing or pressure distribution
- If it is a new socket that the amputee could be expected to acclimitise to, much like a new pair of shoes (but hopefully without the blisters!)
- Potential areas of pain / discomfort that should be further assessed are:
- TTA: The anterodistal tibia. Excessive pressure on the front end of the tibial remnant could indicate a loose socket, where the stump has slid in too far and allowing too much distal weight bearing. IT can also be indicative of insufficient relief over the bony end of the tibia.
- TTA: The distal tip of the patella, particularly in PTB sockets. Pressure on the patella could indicate a loose socket, where the patellar shelf is pressing against the patella iteself, rather than the patellar tendon. The patellar shelf could also be too large (height or amount it bulges in).
- TTA: Distal, anterodistal, or posterodistal stump, where the pain can sometimes be different from 'pressure' pain. This can sometimes occur if the socket is too tight, and the calf muscles are pushed upward as the stump sinks in with weight bearing. The pain can be caused by skin & muscle stretching across the bottom of the stump or over the bony end of the tibia. On examining the stump you may not always see any signs of end-bearing or excessive pressure at the site of pain.
- TTA: The head of fibula. This can be indicative of insufficient relief, or again, a loose socket where the fibular head is not sitting in the relief space.
- TTA: Femoral condyles, particularly in PTS prostheses. This could indicate that the moulding of the supracondylar suspension is too tight, or that the socket is too tight and the suspension is gripping the condyles rather than sitting above them.
- TFA: Perineum / Pubic ramus. Excessive pressure or pain here (in absence of an adductor roll) could indicate the medial socket wall is too high. Ensure this is also checked with the patient shifting weight onto the prosthesis, so the limb becomes slightly adducted.
- TFA: Perineum / Pubic ramus. Ensure the ischial tuberosity is sitting correctly on the posterior brim of quadrilateral sockets, and has not slipped forward to sit inside the socket. A forward sitting tuberosity can indicate a loose socket, or insufficent anterior moulding. A tuberosity sitting outside the socket or above a roll of flesh could indicate too tight a socket, or an incorrect donning technique.
- TFA: Adductor Longus tendons. In quadrilateral sockets, the AL tendon should sit in the antero-medial corner of the socket.
Pain can also be associated with alignment issues. A prosthesis that is designed on selective loading principles (i.e. loading weight tolerant structures and providing relief over intolerant structures) can cause pain if it is not optimally aligned. The Gait Analysis & Training Portal includes information on prosthetic causes of poor alignment.
Assess the alignment of the prosthesis in standing, with equal weight distribution if possible. Sometimes it is necessary to guide the amputee to the midline, using a mirror to give feedback on posture and position.
- Look at medial-lateral alignment:
- TTA: Is the pylon set in valgus in relation to the socket? Ideally it should be in slight varus to take advantage of the principles of selective loading.
- TTA: Is the foot flat, or raised on one side?
- TTA: Is the foot rotated a few degrees outwards? (Check the amputee has not internally rotated their hip).
- TFA: Is the knee joint at the same level as the intact knee?
- TFA: Does the anterior of the knee joint face forward, in the line of progression?
- TFA: Does the degree of toe-out match the other foot?
- Look at the anterior-posterior alignment:
- TTA: In the absence of contracture, is the foot flat on the floor? Sliding paper under the heel or toe can be used to compare between sides.
- TTA: The socket should be in approximately 5 degrees of flexion, tilted forward in relation to the pylon.
- TTA: Is the knee held in excessive flexion or hyperextension?
- TFA: Is the knee stable in extension?
- A backward lean of the prosthesis could indicate too soft a heel cushion (SACH feet) as well as a lack of dorsiflexion.
- Check the height of the prosthesis. On occasion there may be a prosthesis built slightly shorter (up to 12mm) to make up for lack of active dorsiflexion / foot clearance during swing (e.g. some transfemoral prostheses with single axis knees), but generally they should be fairly close in height, if not the same height.
- Question the amputee as to whether they feel they are standing even.
- Check that bony landmarks are roughly parallel in relation to the ground: tops of patella, greater trochanters, ASIS's, PSIS's, iliac crests, popliteal or gluteal soft tissue folds.
- If unsure, place varying thicknesses of wood or books under the prosthesis or intact limb, to see if subjective or objective assessments of height are improved.
- A prosthesis that appears too long could also mean that the patient is not fully into the socket. Check the prosthesis has been donned and weight bearing areas are seated correctly, or that the socket is not too tight.
- Check the skin / socket boundaries:
- TTA: Check posteriorally for rolls of flesh that could be pinched between thigh and posterior brim as the knee flexes.
- TFA: Check above the medial socket wall for presence of an adductor roll. Rolls of flesh here can become painful if pinched between the socket brim and pubic ramus. An adductor roll could indicate incorrect donning, or the medial wall is too low.
- TFA: Check for any overhanging flesh on any other sides of the socket brim.
- TFA: For Ischial Containment Sockets, check that the posteromedial corner actually covers the ischial tuberosity.
- TFA: In the absence of contractures, can the amputee extend their stump, and flex it to 90 degrees?
Suspension
It is important that the prosthetic suspension is adequate, so that the risk of friction and abrasions or blisters through movement of the socket against skin is minimised.
The same methods of assessing the suspension can be used regardless of the type of suspension. Check the amount of drop off by asking the amputee to hitch their hip, raising the foot from the floor in a vertical manner, without flexing the knee.
- TTA: Mark a reference point on the sock or liner with tape, chalk, or other means. For example, across the posterior brim or the socket. Assess how much the prosthesis drops, or pistons, as the amputee lifts their limb and then returns to weight bearing. Pistoning of greater than 1cm may mean the suspension needs adjustments.
- TFA: Palpate the ischial tuberosity. Assess how much the prosthesis drops, or pistons, as the amputee lifts their limb and then returns to weight bearing.
- Unpleasant sounds due to expulsion of air as weight is taken could indicate the valves, suction, or sleeves are not maintaining a seal, and the prosthesis is dropping.
You should also test that the suspension method fits correctly:
- TTA: If there is a suprapatella cuff, does it sit snugly over the top of the patella, and not slide off as the foot is raised?
- TTA: If there is supracondylar suspension, does it sit snugly over the upper portions of the femoral condyles?
- TTA: Can locking pins be easily engaged?
- TFA: Do pelvic bands sit on the pelvis, not the waist?
- TFA: Do pelvic bands silesian belts adequately support the prosthesis and control against rotation or abduction in swing?
- Is the suspension methods at it tightest or loosest, meaning it may not cope with volume changes while the prosthesis is being worn, which may require a short term adjustment to the suspension?
- Do sleeves maintain a seal, as appropriate?
Walking
Ability to assess dynamic fit and alignment is sometimes dependent on the amputees mobility level. Further adjustments may be required as their mobility level improves, and the type of aid changes. Observe any gross gait deviations, or excessive pistoning. Question the amputee again on any areas of pain or discomfort. Judgements made are usually based on the results of the full assessment, for example, is the pain new, or pre-existing? Is that particular gait abnormality due to lack of skill or experience on the part of the amputee, or due to a prosthetic fit or alignment issue? Verbal feedback or manual guidance can sometimes be used to help eliminate patient-related causes of gait abnormalities, but sometimes further assessment is required.
Listen for excessive noise from the socket, or articulated components.
It is also usual that the prosthesis may need adjustment over time, so what looks okay on initial check out may require a review once mobility and balance improves, or the stump further matures.
Depending on the amputees mobility level, assessment can also be made on other surfaces, such as stairs and ramps, where the performance of components can be further checked. For example:
- TTA: Is knee flexion overly restricted during swing phase of stair ascent?
- TFA: Do microprocessor controlled hydraulics provide sufficient knee flexion damping for ramp or stair descent?
After assessing gait (or even earlier if there is a risk of skin or stump damage) remove the prosthesis and reassess the stump. Some redness due to pressure on weight bearing areas is expected. Redness due to friction should be noted, as should marks of pressure over non-tolerant areas, which may indicate that relief of these areas is insufficient. Check the ball of plasticine. It should be compressed, indicating distal contact, but should not be squashed completely flat, which would suggest distal weight bearing.
Actions
Some prosthetics issues identified during checkout can be addressed immediately by the Physiotherapist:
- Extra socks added in loose sockets, although be aware that this also reduces the amount of relief over non-tolerant structures. Also be aware of the effect of adding fabric socks to suction suspension systems, where seals are broken.
- Education / practice of correct donning techniques
Other issues must be referred back to the Prosthetist for resolution. On occasions, if some immediate fixes are required they may be negotiated with the Prosthetist, for example tightening dangerously loose screws. Whether this is permissible sometimes depends on the skill of the Physiotherapist and their knowledge of prosthetic alignment, and their relationship with the Prosthetist. However it is recommended that feedback to the Prosthetist is made so they can check what was done, for example, there are often recommended torque levels for tightening screws.
A Physiotherapist who adjusts a prosthesis must also be aware of any issues of liability, and effects on warranties.